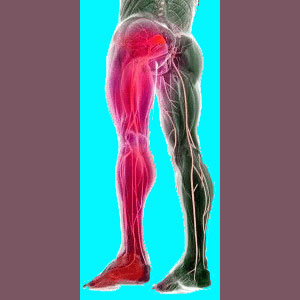
Piriformis leg pain is a common expression of piriformis syndrome, although other diagnoses can be responsible for pain when the leg is mobilized. Leg pain that is experienced in the limb itself is not characteristic of piriformis injury, RSI or muscular imbalance that may be affecting the piriformis muscle. When pain is expressed in the leg, the usual piriformis-related culprit is compression of the sciatic nerve due to muscular spasms. Of course, there are also many, many other explanations for leg pain that might not be related to the piriformis muscle at all.
Leg pain in association with piriformis nerve compression is a type of pseudo-sciatica syndrome. These conditions mimic true spinally-enacted sciatica in every way, except for the fact that they are not sourced in the lumbar/sacral spinal regions. Instead, piriformis-related pseudo-sciatica is caused when the muscle cramps and constricts the fully formed sciatic nerve long after the spinal nerve roots join to form this largest of all human nerves.
This treatise explores the occurrence of piriformis-related leg pain. We will focus on piriformis syndrome as the main causative process, but will detail some alternative possibilities as well.
Piriformis Leg Pain Locations and Expressions
When discussing leg pain, we are not including pain in the hip/sacroiliac/piriformis region higher up that occurs when moving the leg. Instead, we are discussing symptoms that actually occur below the frontier where the leg joins the body, in the limb itself. The usual location for piriformis-related leg pain is in the upper rear of the leg or the upper outer side of the leg. Less commonly, pain might exist in the frontal thigh, rear calf or knee area. Much less commonly, pain may occur in the shin or foot. Since the sciatic nerve is involved, pain might manifest itself virtually anywhere in the leg in rare instances, but the above detailed locales certainly account for the majority of patient complaints.
In addition to pain, patients might also experience any number of additional symptoms in these same areas including tingling, paresthesia, numbness of subjective or objective variety and weakness that often induces functional deficits, such as foot drop. Symptoms tend to progress in this order over time in most patients, although most cases will not reach the degree of functional motor issues, such as the aforementioned dorsiflexion deficit.
Leg Pain Causation
The sciatica nerve is anatomically placed beneath the piriformis muscle in a typical anatomy. However a significant portion of the general population demonstrates abnormities of the sciatic nerve positioning in relation to the piriformis muscle. The sciatic nerve might run directly through the substance of the muscle, in front of the muscle, around the muscle (common in divided sciatic nerves) or in any combination of these irregular configurations.
Regardless of the positioning of the sciatic nerve, the tissue can be compressed if the piriformis goes into spasm and clamps down on the nerve fibers. A compressed nerve will not function correctly and will begin to signal distress to the brain almost immediately. This distress signal is pain and the various other manifestations of symptomology associated with piriformis syndrome.
Piriformis Leg Pain Alternative Explanations
Besides piriformis syndrome, there are many other conditions that might be the true source of virtually identical leg pain expressions. Therefore it is no surprise that piriformis syndrome is often mistakenly diagnosed when the real cause is one of the conditions listed below. Additionally, and on the opposite side of the equation, the following conditions are all commonly blamed for sourcing leg pain that is actually created by piriformis syndrome. Misdiagnosis is a 2 way street when it comes to the mistakes made in diagnosing pseudo-sciatica.
True spinal sciatica can occur due to various conditions impinging on the nerve roots that compose the sciatic nerve. Spinal stenosis and herniated discs are the 2 most commonly implicated mechanisms of nerve root compression, although many others exist.
Sacroiliac disorders can produce pseudo-sciatica and referred leg pain. SIJ pain can be very similar to pain in the piriformis muscle in many patients.
Hip disorders might produce upper leg pain. Hip bursitis and injury can produce strikingly similar pain to piriformis injury and SIJ disorders.
Diabetes is an epidemic in the modern developed world and tends to create various neuropathies that are often not correctly identified for their true nature, especially in the presence of incidental structural explanations in the hip/spine/SIJ or piriformis regions.
Piriformis Pain > Piriformis Symptoms > Piriformis Leg Pain





