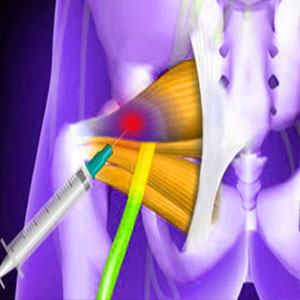
Piriformis injections can be used for pain relief, to reduce spasms or to promote organic healing within the muscle. Injections remain some of the more common diagnostic and treatment practices in the dorsalgia sector of medicine and are especially popular for piriformis pain syndromes. Injections come in different types and levels of invasiveness, ranging from basic subdermal injections to deep muscular injections that are often guided by fluoroscopy for improved accuracy. Regardless of type, injections should always be performed by a licensed physician, even if the substances used do not qualify to be called drugs, such as in the case of prolotherapy.
This essay provides a complete overview of the various types of injection techniques that are used to diagnose and treat piriformis pain conditions. We will explain the risks and benefits of various injection procedures to help patients choose the best therapies for their particular needs.
Diagnostic Piriformis Injections
Some injections are geared towards diagnostic evaluation and are often used in cases of piriformis pain or piriformis syndrome. For suspected injury, RSI or other soft tissue pain syndrome that is expressed directly in the muscle itself, anesthetic injections can be given into the substance of the piriformis and if the pain is relieved, then the muscle is usually implicated as the origin of pain. Similarly, when piriformis syndrome is suspected due to muscular spasming and entrapment of the sciatic and/or pudendal nerves, a powerful muscle relaxant or paralyzing agent might be injected into the piriformis in order to see if the cramping ceases and the symptoms are relieved.
Although these practices are relatively effective, they are not always accurate, since the substance used can spread anatomically and might therefore also interact with other potential causes of pain, such as the sciatic nerve, the pudendal nerve, the hip anatomy or the buttocks musculature.
Treatment with Injection Therapy
Piriformis treatment is commonly performed using injections. The typical types of injections therapies included in a piriformis therapy plan might include any or all of the following, depending on the specific diagnosis involved and the particulars of the patient’s symptoms:
Nerve blocks offer the potential for long lasting pain relief by introducing powerful anesthetics into the painful region of the piriformis anatomy.
Muscle relaxants are usually used for piriformis syndrome where the muscle is thought to be in spasm and constricting the sciatic and/or pudendal nerves.
Botox is another popular piriformis syndrome therapy that can paralyze the piriformis muscle preventing compression of any nerve tissue due to cramping or spasm.
Prolotherapy is used for cases of injury or RSI in the muscle itself, as well as some cases of piriformis syndrome, in order to elicit a natural healing reaction. Prolotherapy uses nonpharmacological irritants that cause the body to react with increased healing response.
Risks of Piriformis Injections
All injections demonstrate minimal risks, including infection and exacerbated pain. Most piriformis injections are deeply placed, meaning that they also entail the risk of nerve damage, continued bleeding or more serious deep infection.
The drugs used in nerve blocks and muscle relaxant injections are dangerous and can have regional effects that are somewhat unpredictable, although complications are truly rare.
Botox is a deadly poison and can prove to be injurious or even fatal in rare instances. Botox should always be administered by an expert in its pain management applications for best results and safest outcomes.
Prolotherapy is often administered by people who are not truly quailed to provide injections. Never trust a nonphysician to inject you, even if the substance used is only sugar water or cod liver oil.
The most common negative factors associated with piriformis injections are disappointing results. Some patients demonstrate no improvement, while others only receive extremely short duration benefits that last for a few days or weeks. Some patients suffer more serious complications, although these events are not overly commonplace.
As noted above, investigational injections are not a precise method of evaluating any painful complaint and should never be the sole evidence used to provide a diagnostic verdict.
Piriformis Pain > Piriformis Treatment> Piriformis Injections





