Piriformis sciatica is the typical symptomatic expression of piriformis syndrome. However, technically, the condition should be called pseudo-sciatica, since it comes from a nonspinal source that affects the fully formed sciatic nerve, rather than the formative nerve roots which combine to create the nerve. Sciatica is known to be one of the worst pain syndromes, both in terms of duration and severity. However, the real reason why it enjoys such a fearsome reputation is its uncanny ability to defy a plethora of seemingly indicated treatment options, often enduring for years.
This essay explores the occurrence of pseudo-sciatica pain as a direct result of piriformis syndrome. We will define the symptom set, identify its possible locations and provide information about what causes this terrible burden of pain.
Piriformis Sciatica Defined
Sciatica is a lower body pain syndrome that originates in the spinal nerve roots between L4 and S3. The sciatic nerve is composed of these 5 nerve roots that join together to form this largest of all bodily nerves. Compression of these nerves is what causes most cases of true sciatica. This compression can occur due to herniated discs, spinal stenosis, atypical spinal curvature or vertebral misalignment. A minority of sciatica syndromes might instead be created by chemical irritation of these same nerve roots.
However, sciatica symptoms which are caused by the piriformis muscle do not qualify to be called true sciatica. Instead, these conditions are referred to as pseudo-sciatica, since they mimic true sciatica in every way, but do not originate in the spinal nerve roots. In the case of piriformis syndrome, the compression takes place after these roots have left the spine and combined to form the sciatic nerve.
It should be noted that there are many possible types of pseudo-sciatica, and piriformis-related symptoms are only one of these possible causations. It is impossible to tell sciatica from pseudo-sciatica by symptomology alone and it is difficult to pinpoint the exact cause of both sciatica and pseudo-sciatica in most patients.
Sciatic Nerve Pain Locations
Piriformis syndrome can compress parts of the sciatic nerve or the entire nerve, creating a variable pattern of symptomology that mirrors true sciatica in its possible diversity of locations. Most patients will have pain in the lower buttocks, where the legs join the torso, as well as pain in the upper rear aspect of the leg or the upper, outer side of the leg. Some patients will experience pain in the frontal thighs, knees and/or calves. Less commonly, a few patients may express pain in the ankle or foot.
Patients might have patterned pain that remains very much the same or symptoms that change often. Either type of expressed symptomology is commonplace. For unilateral piriformis syndrome, symptoms will only occur in one leg on the same side as the impinged nerve. For bilateral piriformis syndrome profiles, symptoms will occur in both legs. In bilateral cases, the locations and expressions might be identical, similar or completely different from one leg to the other.
If the patient demonstrates perineal pain, groin pain, genital pain or pelvic pain, there is an excellent chance that the pudendal nerve is being compressed, as well as, or instead of, the sciatic nerve.
Piriformis Sciatica Causation
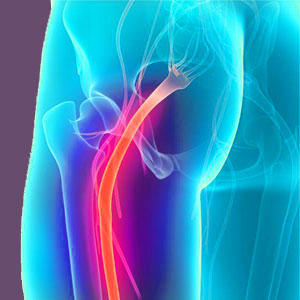
Sciatica symptoms associated with the piriformis muscle are caused when the sciatic nerve is compressed by the muscle as it travels under, in front of or through the piriformis tissue. The sciatic nerve must cross the piriformis muscle as it works its way down the body to form the complex network of nerve tissues in the legs and feet. It is at the juncture with the piriformis that the nerve can suffer compression. Generally, the piriformis is thought to be in spasm, causing it to clamp down on the sciatic nerve, eliciting symptoms.
In a typical anatomy, the sciatic nerve resides beneath the piriformis muscle. However, approximately 17% of the population demonstrates abnormalities in their respective positioning of the nerve in relation to the muscle. Some patients have the nerve travel in front of the muscle. More commonly, part or all of the sciatic nerve travels directly through the substance of the piriformis muscle. In some cases, the nerve actually divides and goes around the muscle on top and bottom, encircling it. Piriformis syndrome can occur in any of these typical or atypical anatomical arrangements, but seems to favor the nerve-through-muscle irregularity based on diagnostic statistics.
What causes the piriformis muscle to go into spasm is usually a major question that can be difficult to answer. Often injury is suspected, but this theory usually does not correlate with patient reports or experiences. In our experience, a very common cause of otherwise idiopathic piriformis syndromes is ischemia of the muscle, causing it to spasm and constrict the nerve. This oxygen deprivation process is invisible and leaves no evidence that can be evaluated without a tissue biopsy from the muscle, followed by special laboratory analysis.
Sciatica has become a major focus on the sites of The Cure Back Pain Network, as well as the niche topic of our very popular website Sciatica-Pain.Org where you can learn all about piriformis-related sciatica in unrivaled detail. We highly recommend reading this resource for patients who want to learn even more about sciatica and how it might relate to piriformis syndrome.
Piriformis Pain > Piriformis Symptoms > Piriformis Sciatica





